COAL MINERS’ LAST LIFELINE
For Justin Smarsh, the clinic at the end of the winding road behind a strip mall in Washington County has been a critical lifeline during his battle with one of the deadliest diseases in mining.
Inside the Lungs at Work center, he was evaluated for the illness that has ravaged his lungs for years and could help him get badly needed benefits to survive.
“They’ll fight for you,” said Mr. Smarsh, who spent nine years in the coal mines of Western Pennsylvania.
Year after year, he breathed in the dust known as silica, one of the most insidious elements in mining — and by far, the most dangerous — leading to the deadliest form of black lung disease.
Three years ago at the age of 39, he was diagnosed with the illness — one of the youngest patients to ever walk into the clinic that screens the new generation of miners for the disease.
Founded 23 years ago with an $88,000 federal grant, Lungs at Work is one of the few clinics of its kind in the nation — a way station that provides the key tests and diagnosis for hundreds of miners in coal country sickened by the toxins that have invaded their lungs.
An investigation by the Pittsburgh Post-Gazette last year found that federal safety experts were alerted to the growing danger of coal dust and the toll that it’s taking on workers, but they failed to crack down on operators who repeatedly exceeded the safety limits.
As the impact of the dust takes a toll on the industry, young miners and older ones are lining up at clinics like Lungs at Work in greater numbers.
Inside the facility, health workers provide checkups and testing that could determine whether the men ever collect the financial benefits and medical care that will last their lifetimes.
Mr. Smarsh, who worked nine years in two Indiana County mines, is among a growing group of miners who have been coming down with the illness after spending much shorter periods underground.
One in five coal workers has come down with black lung in central Appalachia, a stunning number that has sparked protests, rallies and proposed reforms to provide greater protections.
Mr. Smarsh’s condition is so severe that it leaves him gasping for breath and in pain after short walks, unable to carry out the most basic tasks. For years, he has been unable to enjoy his favorite pastimes of hunting and fishing.
After being denied disability payments by the state of Pennsylvania in 2023, he said he’s now fighting to receive the $1,388-a-month federal black lung payments and to relieve his wife, Alicia, of having to work a second job.
The first attorney he consulted to apply for federal benefits told him he probably would not qualify.
“I didn’t know what to do,” said Mr. Smarsh, now 42. So he turned to his wife’s cousin, a fellow miner suffering from black lung who gave him the advice that put him on a new course.
“He said I should call Lungs at Work.”
The small nonprofit in Peters Township is one of just 16 federally funded black lung organizations across the country, most located in the coal fields of Pennsylvania, West Virginia, Kentucky, Tennessee, Ohio and Virginia.
Given the dangers of silica and the battles waged by coal operators to fight paying the benefits, the clinic provides a vital mission to more than 400 underground workers each year.
Week after week, the staff’s three respiratory therapists, a pulmonologist and benefits counselors work with miners to provide their diagnoses and to help them wade through the labyrinth of regulations that can add years to the process.
Some of the men die before they ever collect any money, despite a federal law that requires mine operators to cover monthly benefits to their employees who have the disease.
Deanna Istek, an attorney and Lungs at Work’s CEO, said she was eager to take up Mr. Smarsh’s case when he came to the clinic in 2024.
“We wanted to do everything that we could since his disease is so progressive,” Ms. Istek said. “We met with him and his wife and felt like it was our duty to try everything that we could for them and their family.”
Unlike mining from years ago, Mr. Smarsh was among the young generation of underground workers who had to cut through ever more layers of rock to reach diminished coal seams, kicking up far more silica.
Just months ago, Ms. Istek represented Mr. Smarsh in a hearing before an administrative law judge — the next step in getting him federal black lung benefits after the government denied his initial application in 2024.
With efforts by mine operators to fight the payments, just one in every three applicants ever gets benefits, which range from $793 a month to about $1,587, depending on the number of dependents.
The 16 black lung organizations across the country handling such claims collectively receive $11 million in federal funding, and were first formed in 1979 as an outgrowth of the landmark Federal Coal Mine Health and Safety Act of 1969.
The law was passed after the scourge of black lung among miners first came to the public’s attention in the 1960s.
With a steady increase in federal funding — an amount that was just approved last year for another five years — the organizations have grown collectively to serve nearly 8,000 miners a year in getting their money and medical care.
“It’s an important role,” said Dr. Robert Cohen, a pulmonologist and renowned black lung researcher at the University of Illinois Chicago.
“They do a lot of good work in advocacy and getting the word out to miners about black lung disease and helping diagnose them and apply for benefits.”
Dr. Cohen is also the executive director of the UIC Mining Education and Research Center, which includes one of the federally funded clinics.
“The 8,000 miners we see [in black lung clinics] per year isn’t small given there are only 230,000 coal miners currently working” in the United States, he said.
Nearly all of the black lung clinics are challenged, given the meager $11 million in total federal funding that they receive to take on the battles to help the miners.
Lungs at Work is funded by a $500,000 annual federal grant through the black lung program and roughly $300,000 a year in patient revenue, mostly from insurance payments.
Despite its success, the clinic continues to face its own hurdles, from the rising number of cases caused by silica, to resistance among Pittsburgh-area board certified pulmonologists to work on black lung cases.
The latest effort by mining companies to fight a new rule that forces them to cut down on the amount of silica dust that workers can be exposed to during a shift only added to the list.
“I’ve always felt like I was fighting an uphill battle all the time,” said Lynda Glagola, who founded Lungs at Work in 2002.
She was pushed to launch the clinic after Canonsburg Hospital shuttered its own black lung treatment center, leaving a void for miners in the region.
A respiratory therapist, Ms. Glagola had worked in the hospital’s black lung clinic starting in 2000, and could not bear to watch it go away, she said.
Raised on a farm in north central Ohio, in the two years she worked with the miners who came into the clinic, Ms. Glagola found herself unexpectedly familiar with miners’ approach to life.
“They’re not afraid of hard work and are straightforward with you,” she said. “Even though I’ve still never been in a coal mine, I just felt internally I truly connected to miners from my farming background.”
A member of a devout Baptist family, Ms. Glagola, 69, had intended to become a missionary.
It was not long after working with the miners in the hospital’s black lung clinic that she realized: “God created my mission right here in coal country in Western Pennsylvania.”
Dr. David Celko, a pulmonologist at the hospital who helped Ms. Glagola start the clinic, said it was an easy decision for both of them.
“I do this because of my heritage,” said Dr. Celko, 75, who retired a decade ago but continues to treat miners at the clinic. “My grandfather and uncles worked in mines in Harwick, Harmar and Russellton — mines that are all closed now. I do this to give back to the community.”
Ms. Glagola figured out quickly after opening the clinic that she needed to learn how to do more than just use her skills as a respiratory therapist.
Leaving miners to fend for themselves as they navigated the complex system set up to apply for black lung benefits was going to take expertise she did not have.
With limited funding to hire someone to help, Ms. Glagola said she “just went out and got training to learn how the system works.”
Before taking over as CEO in 2024, Ms. Istek played a much different role: She represented coal companies at the initial hearings that decide whether coal miners qualify for black lung benefits.
For years, she and Ms. Glagola opposed each other in nearly 100 cases, with Ms. Istek winning just a handful.
“She was very good in those hearings,” Ms. Istek said, noting miners can represent themselves, or enlist the help of a layman to represent them like Ms. Glagola. “But most lawyers don’t have the medical background she does.”
Ms. Istek said representing the coal companies as they fought against miners trying to get benefits took the “passion” out of the work that drove her into the legal profession.
Word of the clinic’s work has spread among miners in the region.
Joe Phillips, 76, could have traveled to a clinic much closer to his home in West Virginia, but he drove more than two hours with his daughter, Carrie, 42, to Lungs at Work because of the service and reputation.
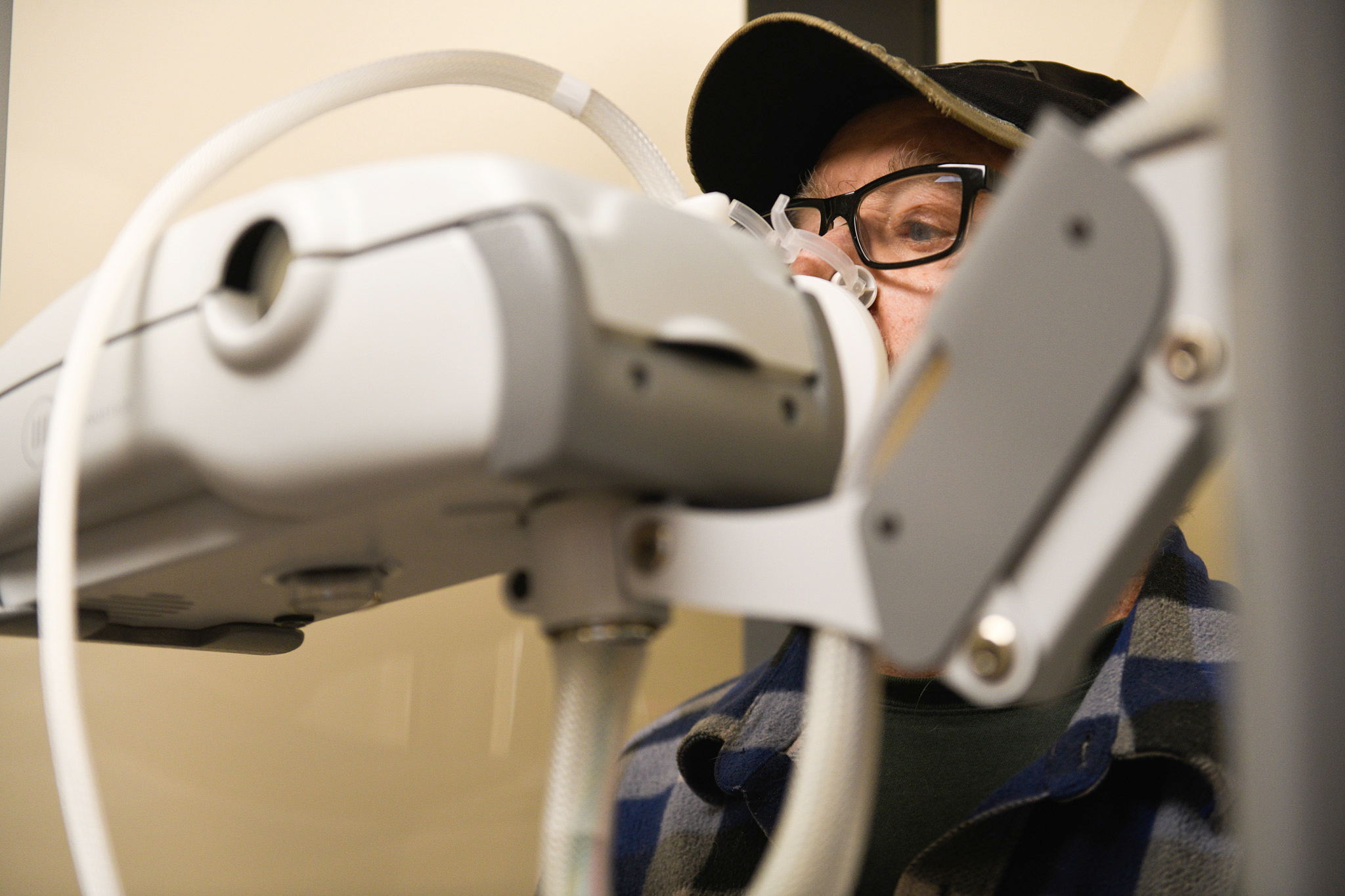
After arriving the first time, he endured an hourlong trio of tests designed to demonstrate his body’s ability to process oxygen.
One of the clinic’s respiratory therapists, Erica Wysocki, explained each test to Mr. Phillips, all of which involved blowing into a machine that would read how well his lungs were working.
Before the first test, known as Forced Vital Capacity, she warned him that his most difficult task might be to refrain from coughing.
The first three tests proved unusable because he couldn’t stop coughing.
“How are you feeling?” Ms. Wysocki asked.
“Oh, I’m OK, I guess,” said Mr. Phillips, wearing a faded ball cap that read “RETIRED MINER” on the front.
It would eventually take 13 tries to get the results needed for his application for benefits.
He also sat through a battery of questions about his medical history with Dr. Celko before being sent for a chest X-ray at a nearby outpatient clinic. It could take several weeks before his diagnosis is reached.
Although he began feeling shortness of breath over a decade ago, Mr. Phillips — who worked in nearly 20 mines during his career — said it was the last three years when it truly began to impact his life.
“I used to walk in the woods for four or five hours hunting roots [like ginseng] only stopping to dig up a root,” he lamented. “But now I can’t walk four or five minutes.”
Mr. Smarsh, who is 34 years younger than Mr. Phillips, said he knows that feeling well.
“It’s the daily exhaustion. That’s the worst,” he said.
While Mr. Smarsh waits for the outcome of his own application for black lung benefits, his wife said his diagnosis has already had a direct impact on their youngest of two sons, Toby, 19, who works as a construction excavator.
“This discouraged our youngest from going underground,” she said. “He’d seen the dollar signs and wanted to work in a mine.
“But now he’s seen what happened to his daddy.”